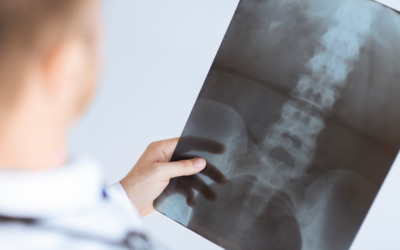
As a physician working with elderly patients, one of the most challenging and rewarding experiences is helping them cope with the pain associated with spinal stenosis. Spinal stenosis develops over time as bones age, discs narrow due to wear and tear, ligaments thicken, or sometimes continues to increase due to injury or other medical conditions. When symptoms of advanced spine stenosis become evident in an individual’s limbs or back because this leads more often than not to great deal of discomfort and distress for those involved. As a healthcare professional it’s important that our seniors understand that despite whichever stage their condition may be at there are many effective treatments available today; providing relief from potentially severe chronic levels of pain and possibly bring about permanent improvement in overall functioning on daily basis activities…
As a general rule, advanced spinal stenosis in the elderly occurs when the spaces within the spine narrow, causing pressure on the nerves and spinal cord. Symptoms include severe pain, numbness, and weakness in the extremities. Treatment options include physical therapy, pain management, and surgery.
If advanced spinal stenosis is an issue for you, let me help you with some valuable insight. With over 30 years of experience in chiropractic practice and training in ergonomics, I’ve authored a book on posture, appeared on national television, and created several solutions to improve sitting comfort and posture. Moreover, I have successfully crowdfunded a project for ergonomic seat cushions.
What is considered severe spinal stenosis?
Severe spinal stenosis refers to a significant narrowing of the spinal canal or the spaces within the spine where nerves and the spinal cord travel. This narrowing can cause compression of the nerves and the spinal cord, leading to pain, numbness, tingling, muscle weakness, and, in some cases, loss of function.
Spinal stenosis is generally categorized as mild, moderate, or severe, depending on the extent of the narrowing and the resulting symptoms. Severe spinal stenosis is typically characterized by:
- Marked narrowing of the spinal canal: Imaging studies, such as MRI or CT scans, may reveal a significant reduction in the size of the spinal canal, nerve root canals, or intervertebral foramina (the openings through which nerves exit the spine).
- Severe symptoms: Patients may experience intense pain, numbness, weakness, or other neurological symptoms in the back, neck, arms, or legs. These symptoms can significantly impair daily activities and quality of life.
- Unresponsiveness to conservative treatments: Severe spinal stenosis may not respond well to non-surgical treatments, such as physical therapy, medications, or injections. In such cases, surgery may be recommended to relieve pressure on the nerves and spinal cord.
It is essential to consult a healthcare professional for an accurate diagnosis and appropriate treatment plan if you suspect you have spinal stenosis.
What is the newest treatment for spinal stenosis?
In addition to traditional treatments like physical therapy and medication, there are some exciting new advancements in the world of spinal stenosis care. One such treatment is the minimally invasive lumbar decompression (MILD) procedure. This innovative technique allows for the removal of excess ligament tissue causing the stenosis without the need for a major surgery. Other advances include regenerative medicine options, such as stem cell therapy and platelet-rich plasma injections, which aim to promote healing and improve spinal function.
Another cutting-edge treatment option for spinal stenosis is the use of stem cell therapy. Stem cells have the unique ability to differentiate into various types of cells, including those that make up spinal discs, ligaments, and bones. Through injection or implantation, stem cells can regenerate damaged tissue and improve spinal function, treating the underlying cause of spinal stenosis.
Further research is needed to determine the long-term effectiveness and safety of these new treatments. However, the development of these advanced therapies provides optimism for a better prognosis for individuals suffering from spinal stenosis, improving their quality of life and reducing their dependency on conventional pain medication.
Spinal stenosis and walking problems
Walking problems are common among patients with spinal stenosis, as the compressed nerves can cause pain, weakness, and numbness in the legs. To combat these challenges, I often recommend that my patients focus on spinal alignment and maintaining a balanced and strong core. This approach not only alleviates pressure on the nerves but also provides better support for the entire body during movement.
All Day Comfort & Support
Walking problems related to spinal stenosis can include:
- Pain: People with spinal stenosis often experience pain in the lower back, buttocks, legs, or neck, which can make walking difficult. This pain can be sharp or a dull ache and typically worsens with activity, such as walking or standing for long periods.
- Numbness and tingling: Spinal stenosis can cause numbness, tingling, or a “pins and needles” sensation in the legs or feet, making walking uncomfortable or challenging.
- Muscle weakness: As spinal stenosis compresses the nerves, it can lead to muscle weakness in the legs. This weakness can cause difficulty lifting the feet, stumbling, or problems maintaining balance while walking.
- Claudication: Neurogenic claudication is a common symptom of lumbar spinal stenosis. It manifests as pain, cramping, or fatigue in the legs that worsens with walking or standing and is relieved by sitting or leaning forward. This can significantly impact the ability to walk or perform daily activities.
- Gait disturbances: Spinal stenosis may lead to changes in a person’s walking pattern, resulting in an unsteady or irregular gait.
If you suspect you have spinal stenosis or are experiencing walking problems, it is essential to consult a healthcare professional for a proper evaluation and diagnosis. Treatment options for spinal stenosis can vary depending on the severity and location of the stenosis and may include medication, physical therapy, lifestyle changes, or surgical intervention in more severe cases.
Stenosis in a 90-year-old
Age shouldn’t be a barrier to comfort and mobility. For older individuals experiencing spinal stenosis, I emphasize the importance of a comprehensive approach, including gentle exercise, regular chiropractic adjustments, and pain management strategies. In some cases, assistive devices like canes or walkers can provide additional support and stability, helping these seniors maintain their independence.
Stenosis can occur in various areas, such as the spinal canal, arteries, or heart valves. In a 90-year-old, common forms of stenosis may include:
Spinal stenosis: This occurs when the spinal canal narrows, compressing the nerves and causing pain, numbness, or weakness in the legs or back. Treatment options may include pain management, physical therapy, or in some cases, surgery. However, the risks and benefits of surgery should be carefully weighed for elderly patients.
Aortic stenosis: This is a narrowing of the aortic valve in the heart, which can lead to reduced blood flow and shortness of breath, chest pain, or fainting. Treatment options may include medication or valve replacement. For a 90-year-old, the least invasive option (TAVR – transcatheter aortic valve replacement) may be considered if the patient is deemed suitable.
Carotid artery stenosis: This refers to the narrowing of the carotid arteries, which supply blood to the brain. It can increase the risk of stroke. Treatment options for elderly patients may include lifestyle modifications, medication, or a procedure called carotid endarterectomy or stenting, depending on the severity and patient’s overall health.
Management of stenosis in a 90-year-old patient will depend on various factors, including the patient’s overall health, the severity of the condition, and potential risks associated with treatment options. It is essential to consult with a healthcare professional to determine the most appropriate course of action.
Severe spinal L4-L5 symptoms
The L4-L5 level of the spine is a common area for spinal stenosis, and when it’s severe, symptoms can be particularly troublesome. Patients may experience lower back pain, sciatica, and leg weakness or numbness. Sitting for long periods can exacerbate these symptoms, but there’s a solution! I always advise using an expert-designed ergonomic seat cushion made with a natural latex top and a high-density base layer foam. Memory foam is a no-go, as it lacks pressure support, resilience, and can be toxic and hot when used for extended periods.
I’ve written a complete hands-on review about the best sitting position for sciatica, and here is what I tested best with my sciatica patients.
Understanding Advanced Spinal Stenosis in Elderly Patients: The Role of Disc Degeneration and Canal Stenosis
Advanced spinal stenosis in elderly patients is often due to a combination of factors, including the natural aging process and wear and tear on the spine. Disc degeneration is a primary contributor, as it can cause the spinal canal to narrow, leading to increased pressure on the nerves. This is known as canal stenosis, and it can be exacerbated by other factors, such as bone spurs and inflammation.
In my clinical experience, I’ve found that maintaining proper spinal alignment and a strong, balanced core is essential for reducing pain and discomfort. This is particularly important when sitting, as poor posture can aggravate symptoms by putting additional stress on the knees. I always advise using an expert-designed ergonomic seat cushion made with a natural latex top and a high-density base layer foam to promote proper alignment and reduce pressure on the spine.
Effective Physical Therapy Strategies for Managing Advanced Spinal Stenosis in the Elderly
Physical therapy is a crucial component in the management of advanced spinal stenosis. I’ve found that a tailored program, including stretching, strengthening exercises, and balance training, can significantly improve patient outcomes.
Here are some key strategies I recommend:
- Flexibility exercises: Gentle stretching of the back, hips, and legs can help alleviate stiffness and improve range of motion.
- Strengthening exercises: Building a strong core and supporting muscles can provide better stability and help maintain proper spinal alignment.
- Balance training: As the aging process can affect balance, incorporating exercises to improve coordination and stability is essential for preventing falls and further injuries.
- Use an ergonomic seat cushion:To best address your seating requirements, it’s necessary to concentrate on various factors, with chair adaptation being a significant one. Several methods can be utilized to attain this, including the addition of an ergonomic cushion and lumbar support. These modifications can lessen the load on your back and legs, promoting comfort and proper posture during long periods of sitting. Moreover, ensure your feet are securely on the ground and that there’s enough distance between your chair and workspace. By following these tips, any standard rigid chair can be transformed into an ergonomic retreat that supports long-term health and well-being.
Ergonomic Sitting Aid
An ergonomic seat wedge (shown above) can be applied to align your spine accurately and improve equilibrium. This superior natural latex seat cushion aids in fortifying core muscles while easing stress in other parts of the body, such as the neck and shoulders. Additionally, sitting upright puts less pressure on your hips and knees, as it engages more muscle groups at the same time compared to resting on a soft surface. This upright stance helps prevent stress-inducing habits that individuals may unknowingly develop while working.
Here’s what I’ve learned from my clinical experience: a strong core helps support the spine, while proper alignment can alleviate pressure on the nerves, making sitting more comfortable. One way to achieve this is by using an expert-designed ergonomic seat cushion made with a natural latex top and a high-density base layer foam.
Now, I know what you’re thinking, “Why not just use memory foam?” Well, I’m glad you asked! I never recommend memory foam for a few reasons. First, it lacks pressure support and resilience, meaning it won’t provide the optimal support needed for a healthy spine. Second, memory foam is a toxic material that gets hot when you sit on it for long periods, leading to discomfort and potential health concerns. Instead, I encourage you to look for a cushion with natural latex and high-density foam, which will better serve your needs.
Best Seat Cushion for Spinal Stenosis SupportAxial Ergonomic Seat Cushion® | Seat Chair Wedge
Quick Guide: A 30-Second Summary

All Day Comfort & Support
Product Name
Axial Designs™ Seat Cushion
Price
$149
Warranty
1 Year
Type
Posture Wedge
Top Layer
100% Natural Latex (Molded)
Bottom Layer
High-Density Foam
Top Material
Isometric Grippy Vegan Leather
Bottom Material
Non-Slip Material
Side Material
3D Breathable Fabric
So, how do you find the perfect ergonomic seat cushion? Here are a few tips:
- Look for a cushion that promotes proper posture by keeping your hips, spine, and shoulders in alignment.
- Make sure the cushion is made of high-quality materials, such as natural latex and high-density foam.
- Check for a non-slip bottom to keep the cushion securely in place while you sit.
- Consider a cushion with a removable, washable cover for easy cleaning and maintenance.
Navigating the Complexities of Advanced Spinal Stenosis: A Comprehensive Approach to Improving Patient Outcomes
When it comes to advanced spinal stenosis, a comprehensive approach is necessary to ensure the best possible outcomes for elderly patients. In addition to physical therapy, I recommend exploring the following options:
- Chiropractic care: Regular chiropractic adjustments can help maintain proper spinal alignment and reduce pressure on the nerves.
- Assistive devices: Supportive braces, canes, or walkers can provide stability and help improve mobility.
- Pain management: Non-invasive pain relief options, such as hot/cold therapy or over-the-counter medications, can help manage discomfort.
- Lifestyle modifications: Maintaining a healthy weight, staying active, and practicing good posture can all contribute to better spinal health.
Final Thoughts
Advanced spinal stenosis is a degenerative disease that affects the spine, causing a narrowing of the spinal canal, leading to pressure on the nerves. Elderly individuals are at a higher risk of developing this condition due to spinal degeneration, disc disease, and other factors. The symptoms of advanced spinal stenosis include neurogenic claudication, lower back pain, and weakness in the legs. Physical therapy is usually the first line of treatment, but in advanced cases, spinal surgery or spinal fusion may be necessary.
The lumbar spine is the most commonly affected area, with a frequency of 5-7 out of 11 references, followed by the lower back, with a frequency of 3-5 references. The cervical spine is also affected, but less frequently, with only 1-2 references. Patients with advanced spinal stenosis often require motor-skill exercises, stretching, and resistance training, all of which are commonly integrated into physical therapy programs.
Several treatment options are available, depending on the severity of the condition. Canal stenosis is a particular concern in advanced spinal stenosis, and surgery may be required to relieve the pressure on the nerves. The frequency of spinal surgery is relatively low, with only one reference throughout the context. On the other hand, the use of physical therapy in the treatment of advanced spinal stenosis can be seen in three to five references.
It is crucial to evaluate and monitor the dosage and volume of medications in elderly patients with advanced spinal stenosis, as they are more vulnerable to side effects from medications. Symptoms of advanced spinal stenosis may include muscle weakness, incontinence, and decreased mobility, which can negatively impact an individual’s quality of life. Clinics devoted to multidisciplinary care are now offering more holistic approaches in the management of advanced spinal stenosis.
Sources:
- Deer, T.R. and Kapural, L., 2010. New image-guided ultra-minimally invasive lumbar decompression method: The mild® procedure. Pain Physician, 13(1), p.35.
- Clinchot, D.M., Kaplan, P.E. and Lamb, J.F., 1998. Lumbar spinal stenosis in an elderly patient. The Journals of Gerontology Series A: Biological Sciences and Medical Sciences, 53(1), pp.M72-M76.
- Postacchini, F., 1996. Management of lumbar spinal stenosis. The Journal of Bone and Joint Surgery. British volume, 78(1), pp.154-164.
- Iversen, M.D. and Katz, J.N., 2001. Examination findings and self-reported walking capacity in patients with lumbar spinal stenosis. Physical therapy, 81(7), pp.1296-1306.
- Bernhard, V.M., Johnson, W.D. and Peterson, J.J., 1972. Carotid artery stenosis: association with surgery for coronary artery disease. Archives of Surgery, 105(6), pp.837-840.
- Achenbach, S., Delgado, V., Hausleiter, J., Schoenhagen, P., Min, J.K. and Leipsic, J.A., 2012. SCCT expert consensus document on computed tomography imaging before transcatheter aortic valve implantation (TAVI)/transcatheter aortic valve replacement (TAVR). Journal of cardiovascular computed tomography, 6(6), pp.366-380.