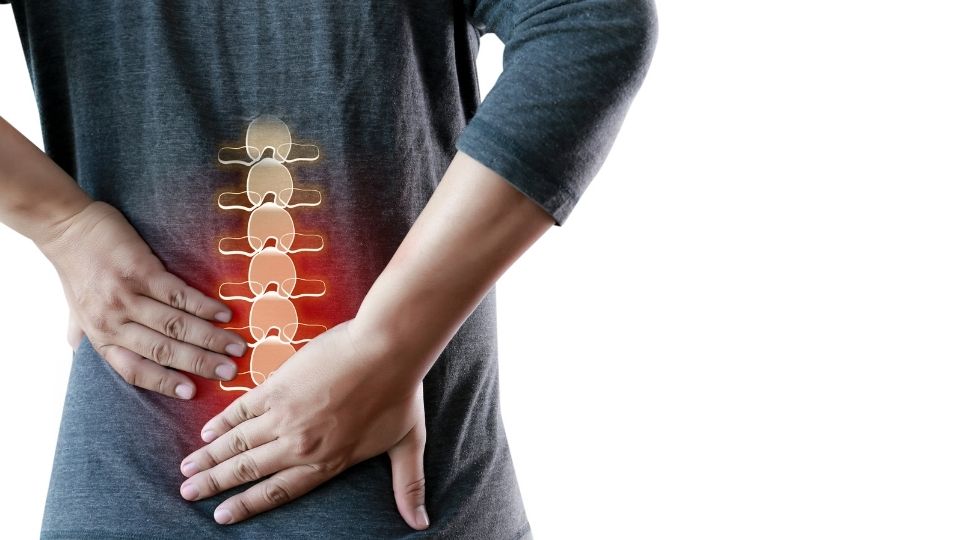
Dr. Woods is here to talk about how you stand up with a herniated disc. This condition is something that many people struggle with, and I know there is a lot of conflicting information*. So, I will clarify and tell you the best way to do it. Ready? Let’s go!
As a general rule, the best way to stand up with a herniated disc is to bend your knees and not lock them while keeping your feet shoulder-width apart. You’ll be able to stand up straighter again without experiencing any additional pain or discomfort.
Standing up correctly is crucial to healing when you have a herniated disc. Besides writing a book on ergonomics and appearing on national television, I’m an expert in ergonomics. Furthermore, I have designed ergonomic seat cushions, orthopedic mattresses, and ergonomic neck pain sleep pillows. If you want better posture and more comfort while sitting, you should get your seating right. It would be my pleasure to provide you with some helpful insights regarding standing with a herniated disc.
Is Standing Good for Herniated Disc?
A herniated disc can be extremely painful, challenging even the simplest movements.* Fortunately, there are things you can do to help ease the pain and improve your quality of life. One of the best things you can do is to try to stand up, move around, or lie down when possible. Sitting (incorrectly) puts more stress on your spinal discs, so standing or moving around can help to take some of the pressure off. (I will show you later in this post how to sit with a herniated disc correctly).
In addition, lying down can also help to relieve pain by taking some of the weight off your spine. Of course, it’s essential to listen to your body and not push yourself too hard. But if you can find ways to move around throughout the day, it can make a big difference in how you feel.
All Day Comfort & Support
Does Standing Make Herniated Lumbar Discs Worse?
A question I often get is, does standing aggravate a herniated disc? Very little evidence points out that standing alone will worsen your pain, although avoiding standing or sitting for long periods is essential. Doctors often recommend that patients with herniated discs keep as active as possible, as this can increase blood flow to the area and speed healing. As a result, even though you may want to avoid standing for long periods, there is little evidence that standing will worsen your herniated disc.
Is It Better to Sit or Lay Down With a Herniated Disc? | Pain Management
Unfortunately, I found in my clinic that there’s no easy answer to this question. While sitting is generally considered better for your back, it’s not necessarily the best position for a herniated disc. Most doctors recommend standing up, moving around, or lying down instead of sitting. The reason is that sitting puts more pressure on your discs, which can aggravate the herniation and cause more pain. So if you’re struggling with a herniated disc, it’s probably best to avoid sitting for long periods. Instead, try lying down or walking around to give your back a break.
Black Friday: 35% Off Today
Typical Delivery 1-3 Days
What Not to Do if I Have a Herniated Disc? | Disc Pain
Many activities can worsen the pain of a herniated disc, including coughing, sneezing, and sitting. These activities put additional pressure on the nerve, which exacerbates the pain. Additionally, bending forward, such as sitting or driving, can worsen the pain. For people with a herniated disc, taking care when engaging in activities that could aggravate the condition is essential. Resting and avoiding activities that put additional pressure on the spine can help to minimize pain and discomfort.
How Long Is Bed Rest for Herniated Disc?
It is vital to get the right amount of rest to recover.* It is always a good idea to get an orthopedic mattress. (I’ve written about this subject and even designed mattresses for a European mattress company.)
A few days of strict bed rest will most likely help ease the pain. However, bed rest should not exceed two days, as this can worsen the pain. Once you are back in your daily routine, you should take frequent rest breaks. This will help your body to heal while also preventing further injury.
How Do I Know My Herniated Disc Is Healing?
Usually, a herniated disk will heal within four to six weeks. However, depending on the severity of the injury and where it occurred, some people may experience relief within a few days. Time is the most significant factor in healing a herniated disk, as the condition often resolves without intervention.
However, depending on your symptoms and the location of the herniation, your doctor may recommend non-surgical spinal decompression to help relieve pressure on the spinal cord or nerve roots. This treatment typically involves wearing a specially designed harness that applies gentle traction to the spine. Spinal decompression can help alleviate pain and promote healing by taking pressure off the herniated disk. Ultimately, treatment aims to help you return to normal activities as soon as possible.
All Day Comfort & Support
What Is the Fastest Way to Heal a Herniated Disc? | Pain Relief
Get Your Sitting Right
To eliminate your back pain, you must identify and avoid the triggers.* The best way is by sitting in a neutral posture at all times; this will reduce sensitivity in those areas of our body that are experiencing discomfort from postural changes like slouching over time due to weariness with continued use.
Anyone who has ever suffered back pain can attest that even the simple act of sitting can be agony if you have the wrong posture. This pain is because sitting causes the low back to flex, putting strain on the spinal discs and ligaments. People with “flexion intolerance” conditions can lead to chronic pain and discomfort. The good news is that you can take some simple steps to reduce the stress on your back when sitting.
First, ensure that you sit straight with both feet on the ground and that your hips are well above your knees. I discovered that this position may restore your spine’s natural curves. This posture may also take some strain off your discs and ligaments. I believe that the best way to achieve this posture is with an ergonomic seat cushion (below). Second, try to avoid slouching, as this will increase the stress on your back.
This design aims to make sitting a dynamic and active experience by constantly changing your posture. This ergonomic seat cushion will help you maintain the natural curve in your low back while avoiding lordosis, which can lead to painful consequences such as ulnar nerve compression or herniated disk disease!
Does Drinking Lots of Water Help With a Herniated Disc?
Maintaining proper hydration is vital for overall health, and it may also help to prevent back pain. The discs in the spine are filled with water, and they rely on a continual supply of water to function correctly. When the discs become dehydrated, they may lose their ability to absorb shocks and compressions. This dehydration can lead to a herniated disc, which can be extremely painful. In addition, staying hydrated helps to keep the spine healthy by removing waste and carrying nutrients to the area. So if you’re looking for ways to prevent back pain, drink plenty of good quality water.
Black Friday: 35% Off Today
Typical Delivery 1-3 Days
Can a Chiropractor Fix a Herniated Disc? | Herniated
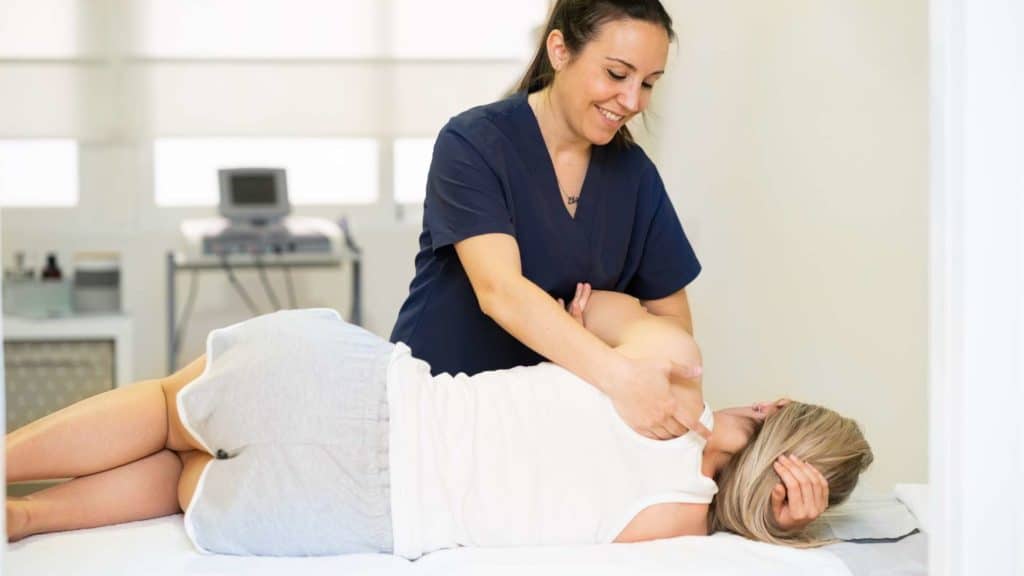
It has been my experience that most people who suffer from a herniated disc can find relief through non-invasive procedures. I believe that non-surgical spinal decompression therapy is one of the most effective conservative methods for treating a herniated disc. Spinal decompression is a non-surgical treatment that uses gentle traction to stretch the spine and relieve pressure on the discs. This type of therapy is effective in reducing pain and promoting healing. Physical therapy treatments such as shockwave or class 4 laser are extremely beneficial as well. It is always best to find a physical therapist who specializes in disc herniation or ‘slipped’ disc treatments.
If you are suffering from a herniated disc, Chiropractic care is an excellent place to start your journey to recovery. A chiropractor can provide spinal decompression therapy and help you heal naturally. Don’t suffer from a herniated disc any longer. Explore your options for treatment today.
Takeaway
When you stand up with a bulging disc, bending your knees is vital to disperse your weight into your muscles and away from your lower back. You don’t want to lock them, and you want to make sure your feet are shoulder-width apart. Doing this will help you stand up straighter without additional pain or discomfort. If you have questions about safely standing up with a herniated disc, speak with your doctor.
Sources:
- MIRZA, S.K. and WHITE III, A.A., 1995. Anatomy of intervertebral disc and pathophysiology of herniated disc disease. Journal of clinical laser medicine & surgery, 13(3), pp.131-142.
- Ito, T., Takano, Y. and Yuasa, N., 2001. Types of lumbar herniated disc and clinical course. Spine, 26(6), pp.648-651.
- Altun, I. and Yüksel, K.Z., 2017. Lumbar herniated disc: spontaneous regression. The Korean Journal of Pain, 30(1), pp.44-50.
- Jordon, J., Konstantinou, K. and O’Dowd, J., 2009. Herniated lumbar disc. BMJ clinical evidence, 2009.